Dog Honking Cough vs Reverse Sneezing: How to Tell the Difference and Act Fast
AI Summary
Dog honking cough vs reverse sneezing is mostly a pattern-recognition problem: reverse sneezing is rapid inward snorting bursts, while cough is a forceful outward event that may repeat and worsen over days. The most important insight is to classify sound direction, recovery quality, and red-flag signs so you know when to isolate, monitor, or seek urgent veterinary care.
Related PawfullyHonest Dog Guides
- Dog Reverse Sneezing When to Worry for deeper red-flag thresholds and episode logging.
- Dog Dehydration Signs when panting, cough stress, and poor fluid intake overlap.
- Dog Kidney Disease Early Signs if chronic illness and appetite drop complicate respiratory episodes.
- Dog Pain Signs Checklist to catch subtle distress behaviors between events.
Dog honking cough vs reverse sneezing is a high-stakes distinction because the same dramatic noise can point to completely different next steps. Reverse sneezing in dogs is often brief and self-limiting, while a persistent dog honking cough can indicate canine infectious respiratory disease, tracheal collapse, chronic bronchitis, or airway irritation that needs medical workup. If you understand the pattern, you reduce panic and improve decisions.
Veterinary sources consistently describe kennel cough as a dry hacking or goose-honk cough that can spread rapidly between dogs, especially in boarding, grooming, and daycare settings. By contrast, reverse sneezing is usually a rapid inward snorting sequence that looks intense but resolves quickly in many dogs. This guide gives you a practical framework for classification, triage, isolation, and escalation so you can protect your dog and avoid delayed care.
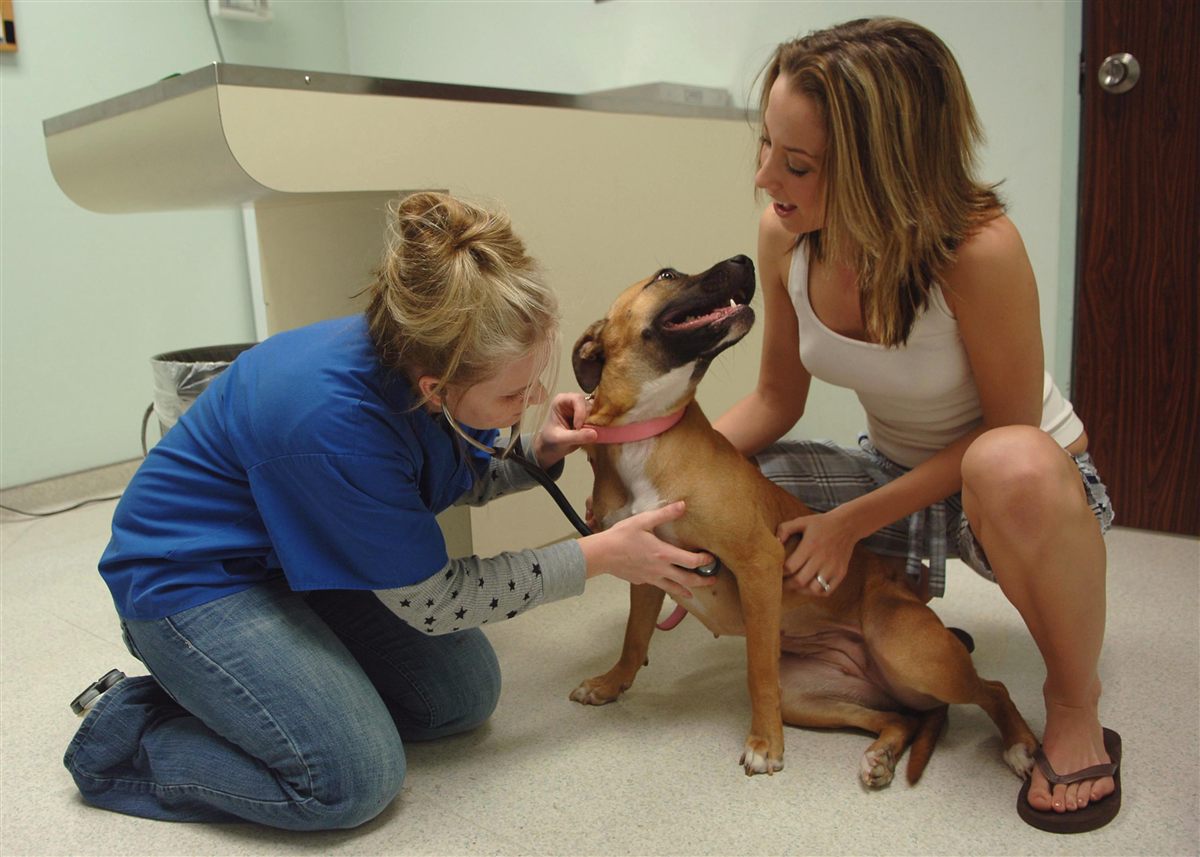
Fast Difference: Honking Cough vs Reverse Sneezing
Use this quick comparison before you over-interpret one noisy event. A single episode is rarely diagnostic, but pattern recognition is still valuable.
| Feature | Honking cough | Reverse sneezing |
|---|---|---|
| Airflow direction | Forceful outward cough | Rapid inward snorting |
| Typical sequence | Cough-cough-gag or retch | Snort bursts with neck extension |
| Duration pattern | Can recur over hours to days | Often seconds to under a minute |
| Contagion concern | Yes if infectious cause suspected | Usually no direct contagion |
| Common trigger | Exercise, pressure on neck, infection | Excitement, irritants, post-nasal drip |
| Between-episode state | May stay irritated or fatigued | Often normal immediately after |
If you cannot classify confidently, assume uncertainty and record a video. Video plus a timeline is far more useful to your veterinarian than a verbal description alone.
Why the Sound Direction Matters Clinically
From a respiratory mechanics perspective, cough is an expiratory event and reverse sneeze is an inspiratory event. That sounds technical, but it is practical: expiratory cough usually points to trachea/bronchi irritation, while inspiratory snorting often points to upper airway reflex irritation around the nasopharynx and soft palate. Different anatomic zones mean different differential diagnoses.
The American Kennel Club notes that kennel cough is commonly identified by a characteristic honking quality and high transmissibility among dogs in shared environments. That transmission profile changes your home plan immediately because isolation decisions matter in the first 24 to 72 hours. On the reverse sneeze side, veterinary guidance from VCA and Merck-style references describes brief paroxysmal events where dogs recover rapidly, especially when triggers are environmental.
Because owners remember sound emotionally, they often miss frequency and recovery trends. Build a log with five fields every time: timestamp, trigger, duration, recovery quality, and exposure history (dog park, boarding, grooming, daycare, visitor dog). In complex cases, this simple log shortens diagnosis time and prevents avoidable antibiotics or delayed imaging.
The best first decision is not medication; it is accurate classification plus isolation if contagion is plausible.
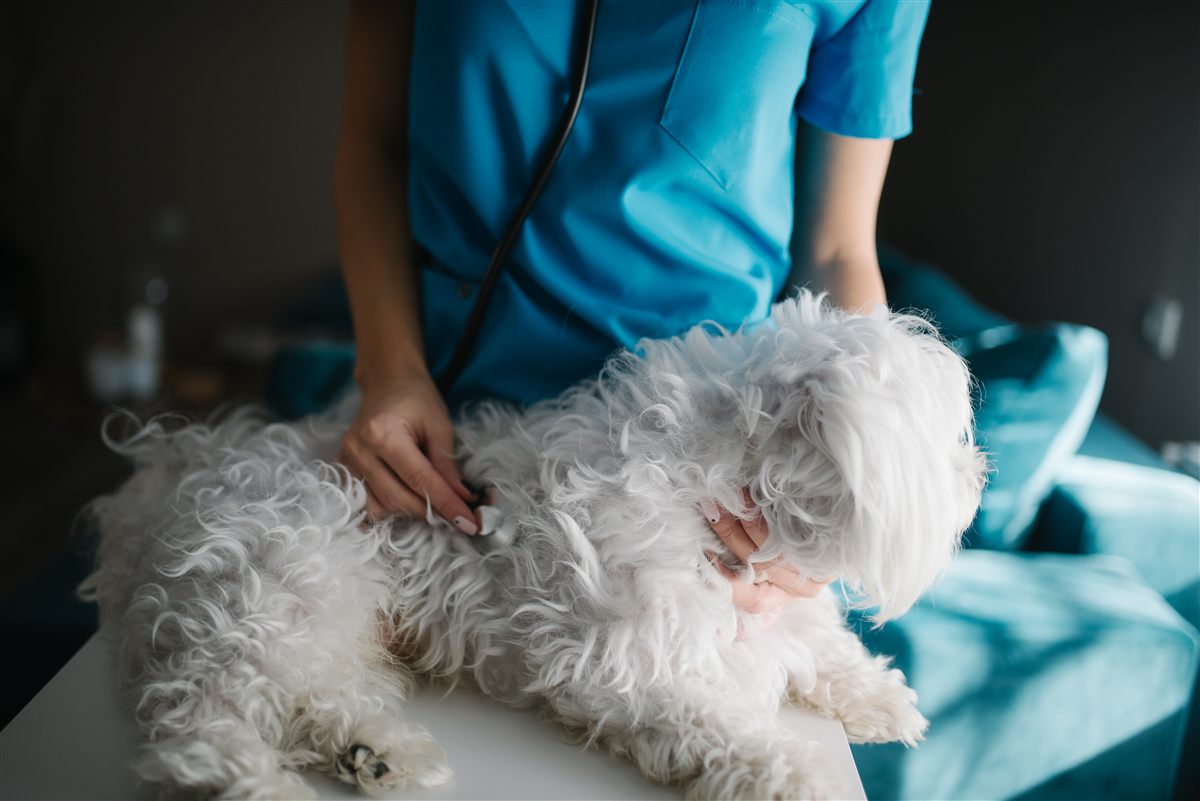
Most Common Causes of a Goose Honk Cough
Owners use the phrase goose honk cough dog for several conditions. These are the major buckets your vet considers:
1. Canine infectious respiratory disease complex (kennel cough)
This is the most familiar cause. It is often a mixed infection picture rather than one single pathogen. Signs include dry repetitive cough, gagging, occasional nasal discharge, and recent exposure to other dogs. Mild cases may stay stable, but some progress, especially in puppies, seniors, or dogs with chronic disease. If infection is suspected, protect other dogs by isolating until veterinary clearance.
2. Tracheal collapse
Small and toy breeds are overrepresented. Cough can worsen with excitement, leash pressure, heat, or weight gain. Many owners report a classic honk at the end of activity bursts. Management usually combines weight control, harness use, trigger reduction, and medications; severe cases may need advanced interventions.
3. Chronic bronchitis or airway inflammation
Persistent cough beyond a short infectious window suggests inflammatory disease, especially when chest radiographs show airway changes. Dogs may have morning cough clusters and post-exertional worsening. A structured treatment plan often includes anti-inflammatory therapy and environment cleanup (smoke, aerosols, dust reduction).
4. Cardiorespiratory overlap and other less common causes
Not every honk is an infection or tracheal issue. Cardiac enlargement, airway foreign material, laryngeal dysfunction, and mass effects can all imitate kennel cough sounds. That is why persistent symptoms deserve objective testing rather than internet-only triage.
What a Reverse Sneeze Episode Usually Looks Like
Reverse sneezing dog treatment usually starts with reassurance and trigger control, not emergency medication. A classic episode includes rapid inward snorts, stiff front-leg stance, neck extension, and brief duration. Many dogs appear fully normal within moments. Episodes may cluster during seasonal irritant peaks or excitement transitions such as door greetings.
The practical challenge is that owners sometimes label every honking event as reverse sneezing because it seems less threatening. Avoid that bias. If episodes are longer, increasingly frequent, or followed by cough and fatigue, classify as uncertain and move to exam mode. In medicine, uncertainty is a valid category; pretending certainty creates risk.
Trigger patterns that support a reverse-sneeze interpretation
- Brief episodes tied to perfume, cleaning spray, pollen bursts, or dust.
- Events during excitement with full normal behavior afterward.
- No fever, no worsening lethargy, no appetite drop, and no persistent cough between events.
Patterns that argue against a benign reflex-only story
- Progressive frequency increase over several days.
- Nighttime waking with repeated respiratory sounds.
- Persistent retching, exercise intolerance, or discharge.
- Any oxygen-compromise sign such as blue-gray mucous membranes.

At-Home Triage Checklist in the First 24 Hours
When owners ask, dog coughing and gagging what do I do now, this is the decision ladder I recommend. It keeps urgency proportional and actionable.
Step 1: Stabilize the environment
Move your dog to a calm, cool area with low stimulation. Switch from collar to harness immediately for walks. Remove aerosol irritants and delay intense exercise. Offer water, but do not force feed if coughing is active.
Step 2: Capture evidence
Record one to three representative videos and write a brief timeline. Include whether sound is inward or outward, whether gagging follows, and how long recovery takes. This evidence often prevents unnecessary repeat visits.
Step 3: Risk stratify
If your dog is bright, eating, and quickly normal between brief events, schedule a routine or next-day consultation. If cough is frequent, sleep-disruptive, or paired with lethargy, request same-day assessment. If breathing distress persists at rest, escalate to emergency care now.
Step 4: Isolate if infection is plausible
No daycare, dog park, boarding, grooming, or shared water bowls until the vet clarifies risk. This single behavior can prevent neighborhood spread if kennel cough is present.
| Observation | Action |
|---|---|
| Single short reverse-sneeze style episode, normal recovery | Monitor and log |
| Repeated dry honking cough, recent dog exposure | Isolate and book same-day exam |
| Cough plus appetite drop or lethargy | Urgent same-day veterinary visit |
| Blue gums, collapse, persistent distress | Emergency hospital immediately |
What Your Vet Will Check and Why
A good respiratory workup is targeted rather than random. Expect history review first because signalment and exposure data narrow the list fast. Your veterinarian will then perform airway-focused auscultation, temperature check, oral exam, and palpation around trachea and cervical structures. In many dogs, this already separates likely infectious cough from other pathways.
When signs persist or severity is moderate to high, diagnostics can include thoracic radiographs, airway pathogen testing, and bloodwork to screen inflammation or systemic disease. Chronic or ambiguous cases may require advanced imaging or endoscopy. This sounds extensive, but precision prevents prolonged trial-and-error treatment that can cost more and delay relief.
Treatment depends on diagnosis and severity. Infectious cases may need supportive care and targeted medication plans. Tracheal collapse management emphasizes harness use, body condition control, anti-inflammatory strategies, and trigger reduction. Inflammatory airway disease can require longer-term management. The correct therapy is diagnosis-led, not sound-led.
Isolation, Contagion Risk, and Household Management
When kennel cough is on the table, household protocols matter. Create a temporary respiratory lane for the symptomatic dog: separate bowls, dedicated leash and harness, separate sleeping area if practical, and hand hygiene between dog interactions. In multi-dog homes, stagger potty breaks and avoid nose-to-nose greetings until risk falls.
Clean high-touch surfaces and fabrics routinely. Ventilation helps. If your dog attends services, notify providers early so they can adjust intake protocols. This is not overreaction; it is basic outbreak control at household scale.
Vaccination status also matters, but vaccines reduce severity and spread risk rather than guaranteeing zero illness. Continue to monitor trend lines even in vaccinated dogs. A mild day one can still become a moderate day three if inflammation ramps.
Prevention Plan for Repeat Events
Long-term prevention is mostly systems design, not one-time intervention. Build a respiratory stability routine:
- Use harnesses to reduce tracheal pressure on walks.
- Keep body condition lean to lower airway workload.
- Reduce indoor irritants: smoke, scented sprays, dusty bedding.
- Adjust exercise intensity in heat and high pollen windows.
- Track event frequency monthly, not just during acute flares.
Pair this with related preventive care from your existing routines: hydration checks from our dehydration guide, behavior stress control from the separation anxiety checklist, and symptom escalation rules in the pain signs checklist. This integrated approach is more durable than isolated reactionary steps.
Finally, set an escalation threshold in advance with your veterinarian. Decide now what number of episodes per day, what duration, and what companion signs trigger same-day visits for your specific dog. Pre-commitment removes indecision when an episode happens at 10 PM and stress is high.
Frequently Asked Questions
Is a honking cough in dogs always kennel cough?
No. Kennel cough is common, but tracheal collapse, bronchitis, and other airway problems can sound nearly identical. Exposure history and exam findings are critical before labeling the cause.
How do I tell reverse sneezing from coughing?
Reverse sneezing is usually an inward snorting run with neck extension and short recovery. Cough is outward, often harsher, and may repeat with gagging. Record video whenever possible.
When is a dog honking cough an emergency?
Any persistent breathing difficulty at rest, blue-gray gums, collapse, or coughing blood needs emergency care. Repeated cough with poor recovery should be seen the same day.
Can collapsed trachea sound like kennel cough?
Yes. The classic goose-honk quality overlaps significantly. Small-breed predisposition and trigger pattern help, but imaging is often needed for confidence.
Should I isolate my dog if it has a honking cough?
If infectious respiratory disease is possible, yes. Avoid close dog-to-dog contact and shared spaces until your veterinarian confirms lower contagion risk.